The BCRI welcomes collaboration with external researchers to undertake research at Bolton Clarke.
All research undertaken at Bolton Clarke must:
-
Include involvement and collaboration with the BCRI from the early stages of project development, and:
-
Be relevant to our communities, staff, organisation and the broader aged care industry;
-
Fill a gap in existing research/knowledge, with the aim of leading to positive change in care delivery;
- Have the approval of the Bolton Clarke HREC and the relevant Bolton Clarke stream business leader (facilitated by BCRI).
All research project applications must undergo a 3 step review process, where appropriate, before commencement. The Research Review and Governance Committee (RRGC) Co-ordinator will facilitate this process and field any enquiries about Research Governance at BC, contact the RRGC Co-ordinator.
For information about whether the project is a Quality Improvement or a research project, please review the following document:
For comprehensive detail about this process and the RRGC please see:
To learn more about the RRGC Process, hear from Dr Rajna Ogrin
Please submit research proposals approximately 4 weeks prior to HREC meeting dates, preferably earlier to engage in a process of codesign with BCRI.
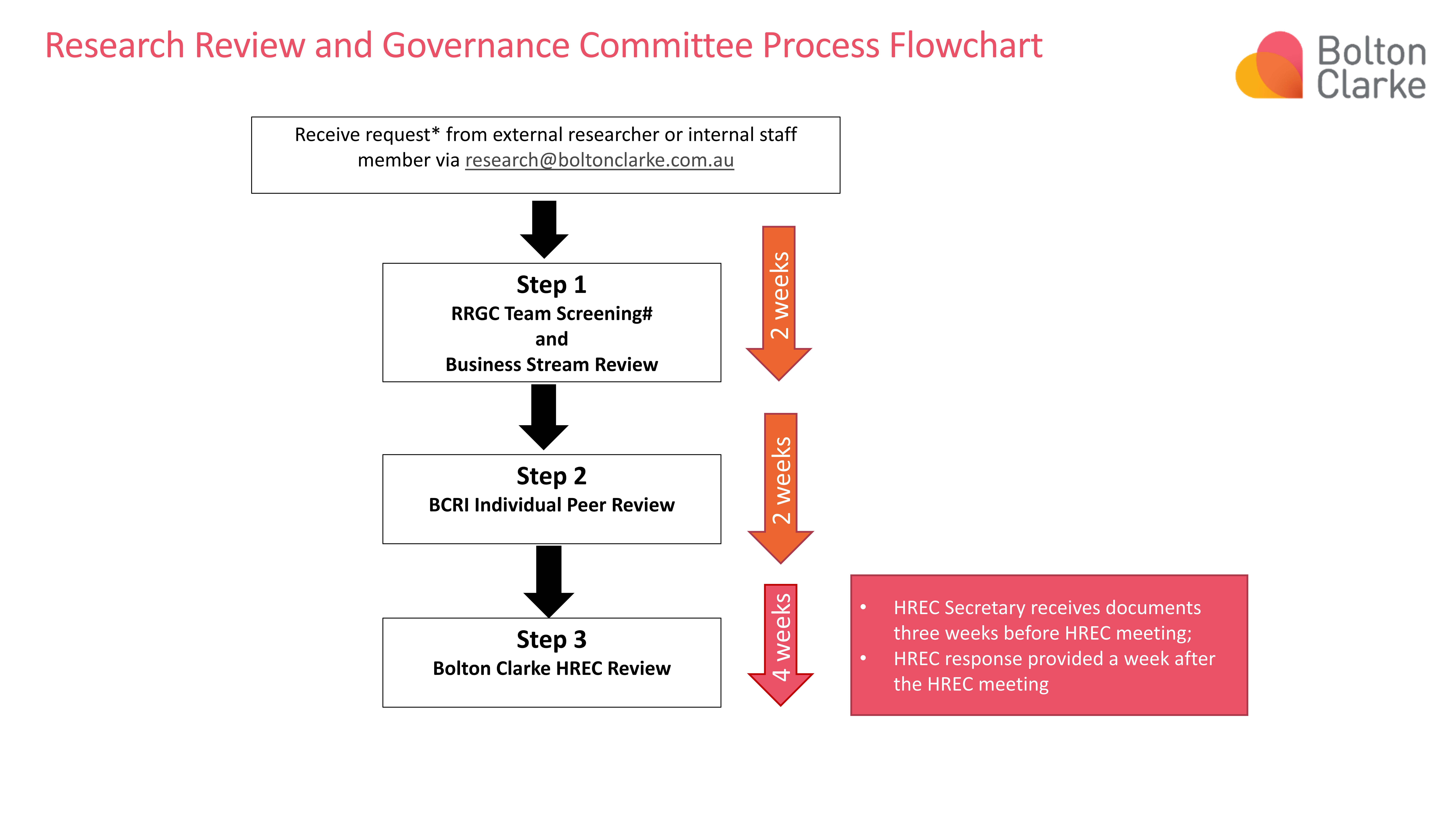
Step 1: Initial review
An initial review of your proposal will be conducted by the RRGC, the relevant Business Stream lead and Head of Research, to assess the proposal for relevance and capacity within the business. Allow 2 weeks to complete this step.
To facilitate this step please send the follow documents to the RRGC Co-ordinator:
Step 2: Peer Review
After RRGC, Business Stream and Head of Research approvals have been obtained at Step 1, your research proposal will undergo peer review by members of the BCRI and relevant experts within the organization. The peer review will be facilitated by the RRGC Co-ordinator and requires 2 weeks.
The following documents will be required for the peer review:
The review process will identify whether the project is suitable to progress to:
- HREC review with no or minimal changes required - applicants will be advised what changes, if any, would be appropriate; or
- requires amendments as advised by BCRI reviewers and re-review by the RRGC Co-ordinator - the review process will continue until the application meets the requirements for HREC submission; or
- not suitable to progress to HREC review - the application cannot proceed to HREC submission.
Step 3: HREC
The RRGC Co-ordinator will facilitate your submission to the HREC and ensure all the required documentation is provided. All documents listed in the HREC Checklist will need to be completed.
Find out more information about the Bolton Clarke HREC
Retirement Living
Independent to low care needsResidential Aged Care
Medium to high care needs